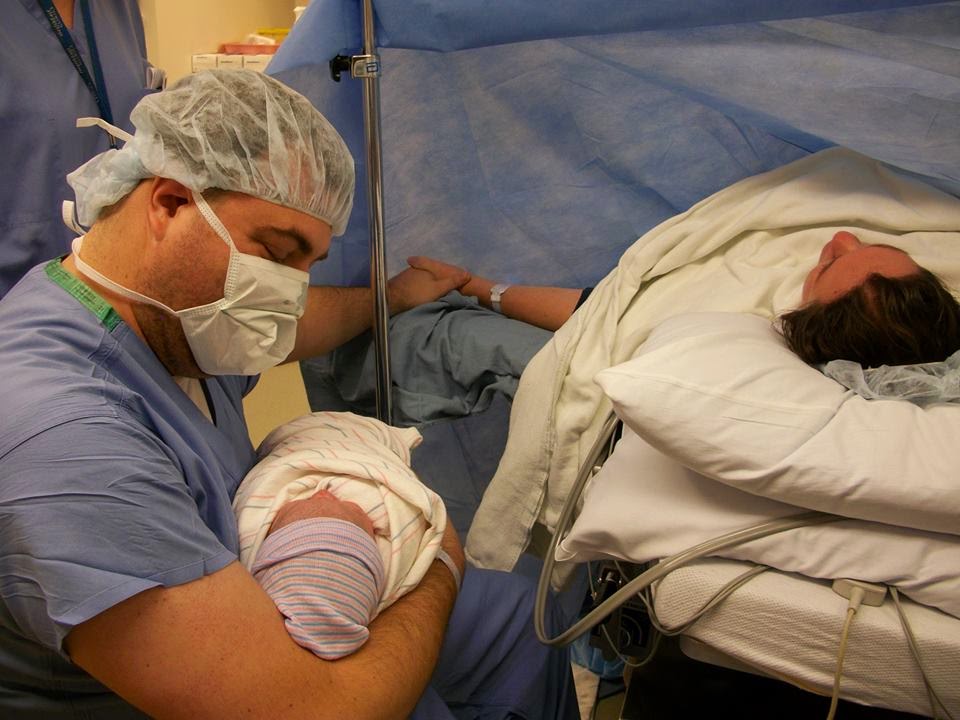
Our guess date came and went. I wasn’t surprised. We went 10 days over with our first, so I was prepared to try to enjoy the wait. I had been especially nesty all weekend- at one point I washed the insides of all of our trash cans. Again.
It was Tuesday night, and I was getting ready for bed thinking “well, it didn’t happen today. Maybe tomorrow.” But I laid awake, unable to sleep, until 1:30 am. I started feeling crampy and having some mild contractions, so decided to take a bath. I had been pestering my husband the last couple weeks with false labor pains and so didn’t feel the need to wake him up just yet. I got into the tub and started concentrating on my contractions. Wow. They were getting pretty regular and strong. So I started timing them and sure enough they were 45 seconds to a minute long and happening every three to five minutes. I woke up my husband and he groggily helped me time contractions. “Yep,” he said, “this is it!”
I texted my doula and told her that it was happening! For real this time! We called my mother-in-law to come and watch our son. Even though it was 3:00 in the morning, she answered partway through the first ring because she had been especially eager and anxious about this birth ever since I told the family that I was hoping for a VBAC this time…
Our first birth ended in an emergency c- section. I had labored naturally for 24 hours and stalled out at 9 ½ cm dilation. My OB diagnosed me with cephalopelvic disproportion, and consequently our 7 lb, 14 oz baby was delivered via c- section. And although I was completely in love with my perfectly healthy and happy newborn son, the surgery and recovery was quite a traumatic event for my husband and me. We had a lot of unanswered questions after his birth. And I lamented for months about what I could have done differently to avoid having the surgery that was so physically and emotionally painful.
So when I became pregnant with my second, a floodgate of thoughts and emotions came up again. I knew that things needed to be different this time. But for some reason, I had a difficult time breaking up with my OB at first. She wasn’t exactly pressuring me to have a repeat c- section, but she definitely wasn’t VBAC supportive. She was labeling me as a “high risk” pregnancy because in her words I “wasn’t able to deliver my first, and he really wasn’t that big”. She made me feel like such a failure!! I got a second opinion from another OB at the same clinic, and she told me that I likely had a narrow pelvis and wasn’t the best candidate for a VBAC. But that she would consider letting me do a TOLAC. The whole thing just didn’t feel right. So I researched. And finally found a solution. I instantly felt better when at 28 weeks I decided to leave the clinic and get onboard with a team of midwives in the twin cities. They were so supportive of my hopes for an unmedicated birth and VBAC! They just “got it”. I loved their philosophy that childbirth is a natural, normal process. Not a medical condition. I had also done some emotional work with a psychotherapist and saw a prenatal chiropractor regularly. I hired a doula. We took a VBAC childbirth class. I felt ready and prepared to have this baby. Well, as ready as I’d ever be.
Our plan was to labor at home until we were sure that we were in labor, then drive to mom’s house in the twin cities and labor there as long as possible until going to the hospital. My mother-in-law arrived around 3:30 am and by then I was doubling over in pain with each contraction. We told her that we were off to my mom’s house, and she seemed surprised that we weren’t going straight to the hospital. I must have looked pretty miserable. But again, in order to increase our chances of a successful VBAC we wanted to stay away from the hospital as long as safely possible. On our way down to the cities, I called my midwife and was still able to form complete sentences and speak clearly. She instructed us that she’d call back in two hours, but that we should of course call her if anything was alarming. We listened to hypnobirthing on the way down. Not sure if it helped, but I figured it couldn’t hurt.
We arrived at my mom’s house around 5:00 am and I moaned and groaned in her jacuzzi tub for about an hour. When the midwife called, my husband answered and held the phone up in the bathroom so that she could hear me. The midwife could tell that it was time for me to head to the hospital and she said she’d head there too and get the room ready for us. It made me feel so safe and secure to know that she would be available immediately upon our arrival. My husband had also been texting and calling our doula and finally got a hold of her around 6:00 am. She was on her way down as well but would be hitting rush hour traffic. “No problem” I thought. I still have a few hours to go, or so I thought…
After a very uncomfortable ride to the hospital (“Turn on the heat!! No- roll down all the windows! Turn on the air conditioning!! I think I’m going to puke!”) we got to the hospital around 6:15 am. I had about five strong contractions just from the parking space to the front door of the building. We checked in and took the elevator up to the birthing floor. The poor security guard in the elevator had to put up with my pacing and groaning the whole ride up. We were quickly escorted to the triage and my midwife was there, smiling at me. What a good feeling! We skipped the admission questionnaire and got right to a cervical check. I was dilated to seven! Hooray!
The contractions were so strong and frequent, I couldn’t catch my breath and I was swearing and roaring as we walked the hallway to my room. I’m sure I looked and sounded pretty pitiful. “What is your plan for managing pain?” the nurse asked me. I was getting another contraction, so growled and hunched over the handrail and said “this”. When we got to the room, she handed me an aromatherapy stick filled with lavender. “To use for pain management” she said. I wanted to jam the stick into her eye. If I could have, I probably would have said something mean to her. Luckily I was unable to talk through the pain. So I held the stick to my nose. And for just a split second the strong scent gave me just a tiny little break. And it helped.
It was about 6:30 am, and the contractions were constant. My midwife was there with us most of the time, getting the room ready, hooking up my IV antibiotics, and coaching me through contractions. She was so smiley and pleasant, and it made me feel so confident that everything was ok. I was really really vocal with this labor, which surprised me. I was snarling and growling and yelling. My husband looked terrified and my doula wasn’t there yet. Luckily our nurse had another great idea. Her and my husband helped me into the shower. I laid my chest on an exercise ball, knees on the floor, hands gripping the legs of a step stool, and my husband sprayed water on my back while the nurse held the monitor on my belly. Almost instantly, I started to feel “pushy”. I had never felt the sensation with my first, and I was excited that I had made it to this stage. It felt good to finally feel a productive push at the end of the fast and furious contractions that were overtaking me.
My doula arrived at about 8:30 am. I was so relieved to see her. I laid on the bed with my husband at my side, the nurse holding the monitor on my belly, and my doula and midwife by my feet. I was dilaIated to 9. I was pretty tense, crouched in the fetal position. My doula tried massaging my back but she noticed right away that I wasn’t into it. I felt overly sensitive to touch. I was even pushing my husband’s hand away.
My midwife helped me open my legs to open my pelvis and “POP!” my water broke pretty dramatically. After that the contractions were nonstop. I was grunting and starting to push, even though I wasn’t quite dilated to 10 yet. For an instant the pain was so sharp that I thought, “I hope that’s not my uterus rupturing”. I knew this was something that I was supposed to be concerned about, but funny thing was that I just knew that it wasn’t going to happen.
Then the antibiotics were stopped. I pushed and pushed for about 20 minutes. My doula suggested that I squat and hold the headrest to further open up my pelvis. I instantly felt the baby start to move down and out of me. But apparently baby’s heart rate was dropping during contractions and a bunch of people came into the room and sort of watched from afar. It felt strange to have an audience, but I was pretty oblivious to it all until my midwife very calmly told me that they were there to monitor the baby’s heart rate- that it was dipping a little bit with each push, but that I should just keep doing what I was doing but that I’d have to lay down again. That I was doing great. The room was dark and quiet, so surprisingly I barely even noticed that they were there because “ouch!” there’s the ring of fire that everyone talks about!
I pushed for another twenty minutes but still no baby. My husband was in charge of putting the oxygen mask on me between pushes to get more oxygen to baby. It was his only job and he kept forgetting to do it. I could tell that he was so nervous and excited. At this point I was frustrated and asking what to do and if I was doing it right and saying that I don’t think I can do this. My doula and midwife told me to try to push deeper, to remain quiet, and push from within. That I could do this. I tried a few more times, but baby wasn’t coming.
For just a split second I thought that I was failing again and baby was going to have to get cut out of me. But that thought quickly left me because everyone in the room was so calm and confident, I was sure that everything was going ok. My midwife was smiling at me and said, “You need to get this baby out. We need you to get it out on the next push, ok?” I pushed hard. Still no baby.
Apparently she did an episiotomy. I didn’t even feel the cut.
Then I pushed again.
I felt a gush and a release.
I heard my midwife ask me if I wanted to catch my baby.
I was dumbfounded, but instinctively reached down and grabbed my warm little baby girl.
Instantly the pain was gone and instead I just swelled up with love and pride.
It worked! It happened! We did it! Our baby girl was perfect!!!
I was hooked up to pitocin and one more push and the placenta was out. I had some 3rd degree tearing and so was stitched up by a surgeon. But I didn’t even notice or care. I felt like superwoman and just held my baby and smiled. I don’t even think I cried. I was just too happy!! Baby nursed like a champ and I was up and walking around just a couple hours after her birth. It was such a wonderful experience and I feel so fortunate to have been given the opportunity for my natural, vaginal birth. And although it didn’t erase the painful memories of my son’s birth, it did give me some peace of mind and spirit to be able to do what I knew I was meant to do.
Tallulah Mary was born on September 24th, 2014 at 9:42 am. She came in at 7 pounds, 12.5 ounces and 19.5 inches.